7 Signs You May Need a Root Canal

At Casas Adobes Dentistry, our team has helped hundreds of patients identify and treat root canal problems before they turned into serious, painful emergencies. We understand that the words "root canal" can cause anxiety, but the truth is that recognizing the warning signs early gives you the best chance of saving your tooth and getting out of pain quickly. In this guide, we walk you through exactly what to look for and what to do if you notice these symptoms.
Why Recognizing Root Canal Symptoms Early Matters
Root canals treat infection inside the tooth. When the soft tissue at the center of your tooth, called the pulp, becomes infected or inflamed, the bacteria can spread fast. Catching the problem early often means a simpler procedure, less pain overall, and a much better chance of keeping your natural tooth.
Waiting too long can turn a treatable infection into a dental emergency. Swelling can spread to the jaw or face, the tooth may become unsaveable, and the overall treatment process becomes more complex and costly. If something feels off with a tooth, paying attention to that instinct is worth it. Still not sure if what you're experiencing warrants a visit? Learn more about whether you need a root canal on our dedicated page.
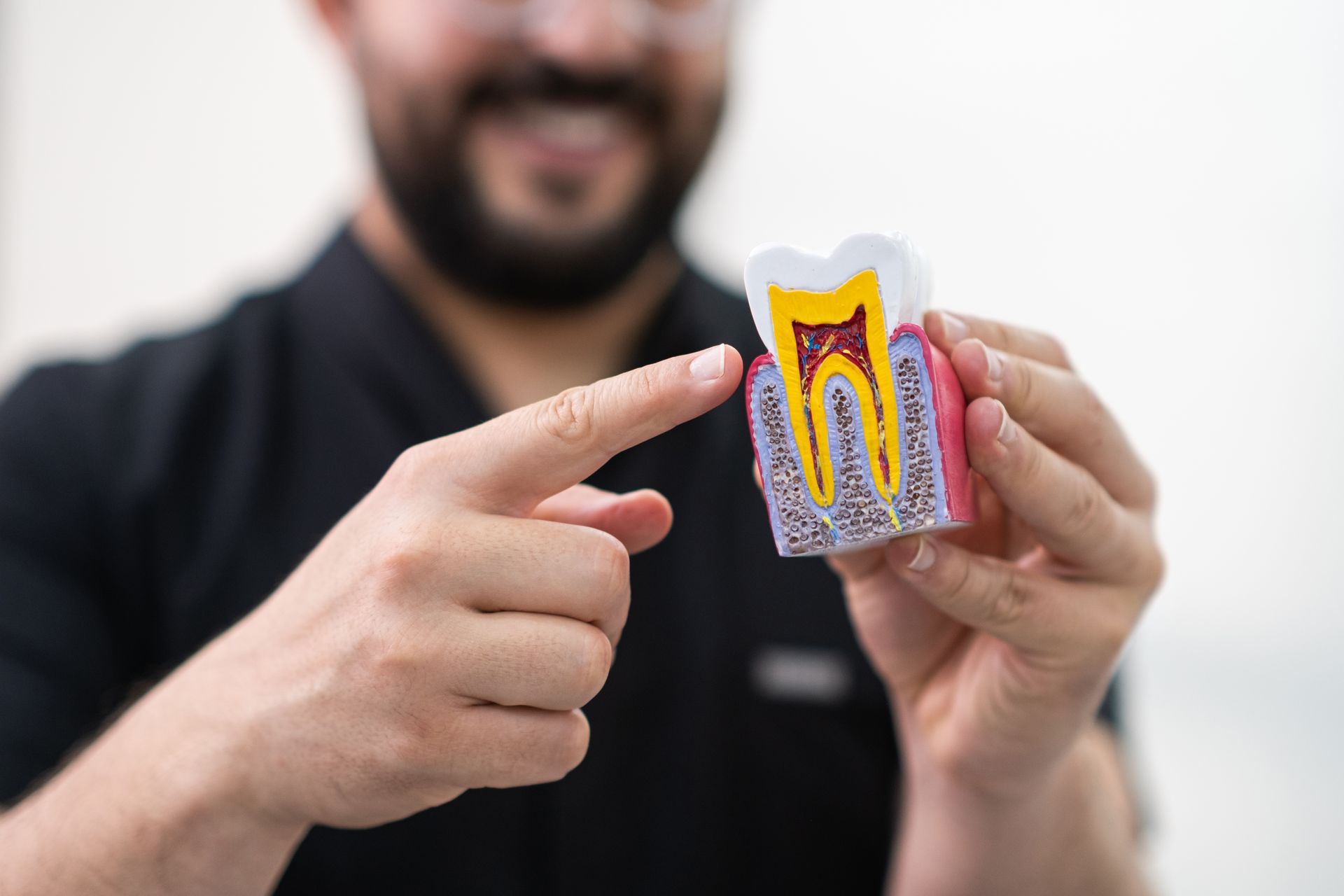
What Is a Root Canal?
A root canal is a procedure that removes infected or damaged pulp tissue from inside the tooth. Your dentist cleans out the canals inside the root, disinfects the area, and seals the tooth to prevent reinfection. In most cases, a crown is placed over the tooth afterward to restore its strength and function.
Despite its reputation, a root canal is designed to relieve pain, not cause it. Most patients report that the procedure itself feels similar to getting a filling. The pain you feel before treatment is the problem. The root canal is the solution.
Common Causes of Root Canal Problems
Deep Tooth Decay
When a cavity is left untreated long enough, bacteria can eat through the enamel and dentin and eventually reach the pulp. Once the pulp is infected, a filling alone won't be enough to fix it.
Cracked or Broken Teeth
A crack in a tooth, even one you can't see, can create a path for bacteria to enter the pulp. This is especially common in back teeth that endure heavy chewing pressure. If you're unsure whether your cracked tooth needs urgent attention, read our guide on whether a cracked tooth is a dental emergency.
Repeated Dental Work on the Same Tooth
A tooth that has been filled or treated multiple times becomes more vulnerable over time. Each procedure puts stress on the tooth structure, and eventually the pulp can become inflamed or damaged even without active decay.
Trauma or Injury to the Tooth
A hard blow to the mouth, whether from a fall, sports injury, or accident, can damage the pulp even if the tooth looks intact on the outside. Internal damage from trauma may not show up right away, which is why it's important to have any dental injury evaluated.
Untreated Infection
An abscess or infection that isn't treated can work its way into the tooth's root system. Once the infection reaches the pulp, the only options are root canal treatment or extraction.
7 Signs You May Need a Root Canal
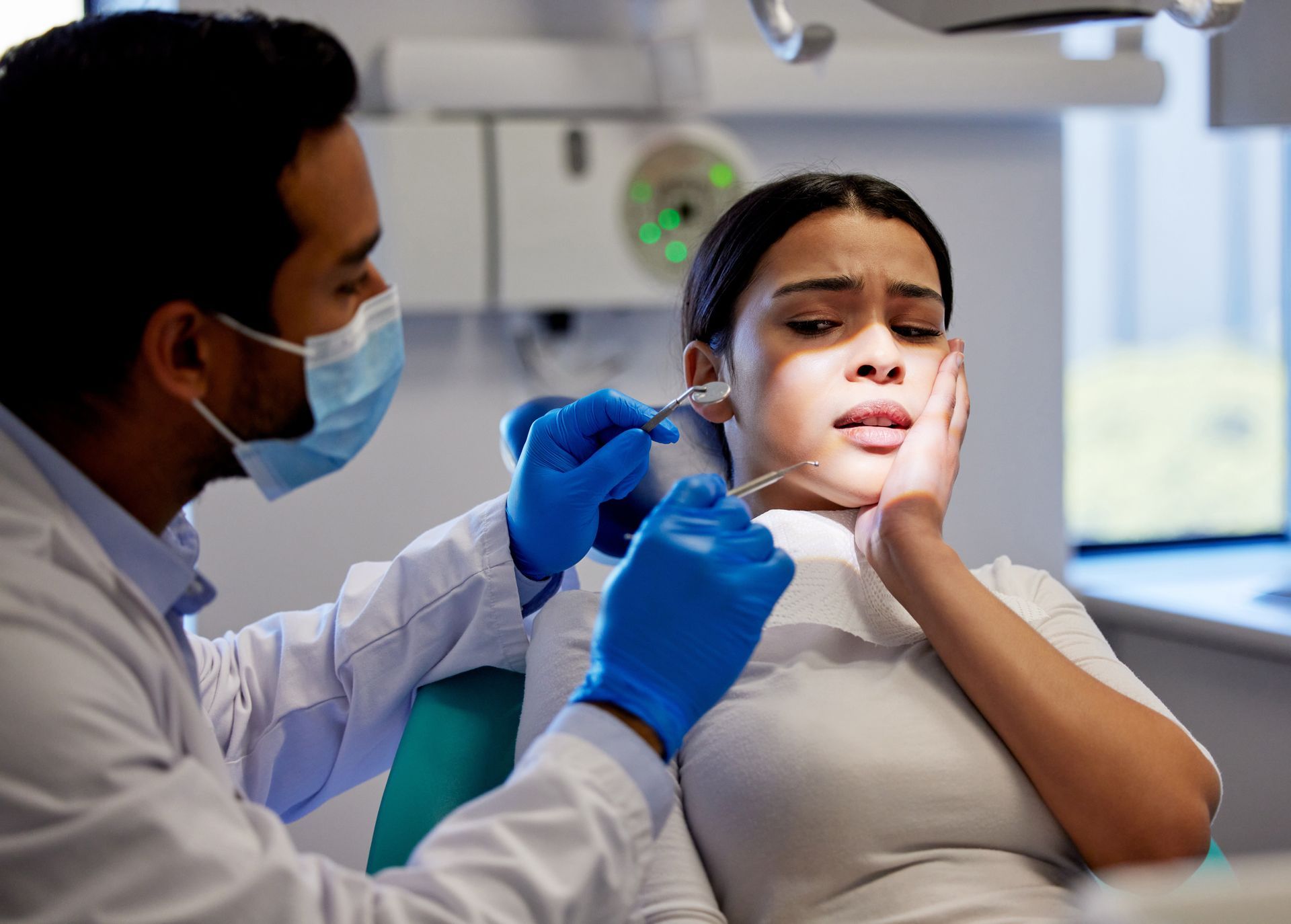
1. Persistent Tooth Pain
Pain that comes back regularly, lingers throughout the day, or throbs even when you're not eating is one of the strongest signs that something is wrong inside the tooth. This type of pain often originates deep in the tooth and can sometimes radiate to the jaw, ear, or surrounding teeth. Over-the-counter pain relievers may dull it temporarily, but they won't fix the underlying problem.
2. Sensitivity to Hot or Cold That Lasts
It's normal for teeth to briefly react to hot coffee or cold ice cream. What isn't normal is sensitivity that continues for 30 seconds or more after the source is removed. Lingering temperature sensitivity suggests the nerve tissue inside the tooth may be inflamed or damaged, and it often gets worse over time without treatment.
3. Pain When Biting or Chewing
If pressing down on a tooth causes a sharp jolt of pain, the nerve inside may be inflamed or the surrounding tissue may be infected. This kind of pressure sensitivity makes eating uncomfortable and tends to worsen as the infection progresses. It's a sign you should book a dental exam soon.
4. Swollen or Tender Gums
Localized swelling near a specific tooth is a red flag. The gum tissue around an infected tooth may feel puffy, tender to the touch, or look darker than the surrounding gum. This swelling is caused by the body trying to fight the infection spreading from the root tip into the surrounding tissue.
5. Darkening or Discoloration of the Tooth
A tooth that has turned gray, brown, or noticeably darker than the teeth around it may have internal damage. Discoloration happens when the pulp tissue breaks down and the byproducts stain the tooth from the inside. This is a sign that the nerve may already be dying or dead.
6. Pimple or Bump on the Gums
A small raised bump, sometimes called a gum boil or fistula, that appears near the root of a tooth is often a drainage point for infection. It may come and go, and it might not be painful on its own. But its presence almost always indicates an abscess forming at the root. This needs professional attention right away.
7. Cracked, Chipped, or Deeply Decayed Tooth
Visible structural damage to a tooth, whether from a crack, chip, or large cavity, can expose the inner pulp to bacteria. Not every cracked or chipped tooth needs a root canal, but when that damage goes deep enough to affect the pulp, treatment is necessary to prevent or address infection.
Signs You May Need Emergency Dental Care Instead
Some symptoms go beyond a standard root canal situation and require same-day care from an emergency dentist.
Facial Swelling
Swelling that extends from the gums into the face, jaw, or neck is a serious warning sign. This type of swelling can indicate that an infection has spread beyond the tooth and into surrounding tissues. It should never be ignored or waited out.
Fever or Severe Infection Symptoms
A fever alongside tooth pain suggests your body is fighting a spreading infection. If you also feel generally unwell, fatigued, or have chills, seek care immediately. Dental infections can become life-threatening when they spread to the bloodstream.
Intense Pain That Prevents Sleeping or Eating
Pain severe enough to keep you awake at night or make it impossible to eat warrants same-day dental attention. This level of discomfort typically means the infection or nerve damage has become advanced.
Trouble Swallowing or Opening the Mouth
Difficulty swallowing or limited ability to open your mouth alongside dental pain is a medical emergency. These symptoms can indicate a deep space infection that requires urgent intervention beyond routine dental care.
What Happens If You Ignore These Symptoms?
Infection Can Spread
A tooth infection doesn't stay contained to one spot. Bacteria can travel through the root tip into the jawbone, spread to adjacent teeth, and in serious cases reach the neck, sinuses, or bloodstream. The longer you wait, the greater the risk.
Pain Often Gets Worse
Root canal symptoms rarely improve on their own. What starts as occasional sensitivity can escalate into constant, severe pain within days or weeks. The infection has nowhere to go except deeper.
Tooth Loss May Become More Likely
A tooth that might have been saved with timely root canal treatment can become unrestorable if the infection destroys too much of the surrounding bone and tissue. Extraction then becomes the only option, which leads to additional costs and procedures for tooth replacement.
Treatment Can Become More Complex
Early-stage root canal treatment is typically straightforward. A tooth that has been infected for months may require more extensive work, additional appointments, or even surgical intervention if the infection has spread into the bone.
How a Dentist Confirms You Need a Root Canal
Dental Exam
Your dentist will visually inspect the tooth and surrounding gum tissue, looking for signs of swelling, discoloration, damage, and gum boils. They'll also ask about your symptoms, how long they've been present, and what makes them better or worse.
X-Rays or Digital Imaging
X-rays allow your dentist to see inside the tooth and the bone around the root tip. Darkening at the root tip, known as a periapical lesion, is a clear indicator of infection. Digital imaging gives a more detailed, immediate view of what's happening below the surface.
Pulp and Sensitivity Testing
Your dentist may test how the tooth responds to temperature or light pressure. A tooth that doesn't respond at all to cold stimulus may have a dead or dying nerve. A tooth that reacts and then keeps hurting for a prolonged period often has inflamed pulp tissue. These tests help confirm whether the pulp is still healthy or needs to be removed.
What to Expect During Root Canal Treatment
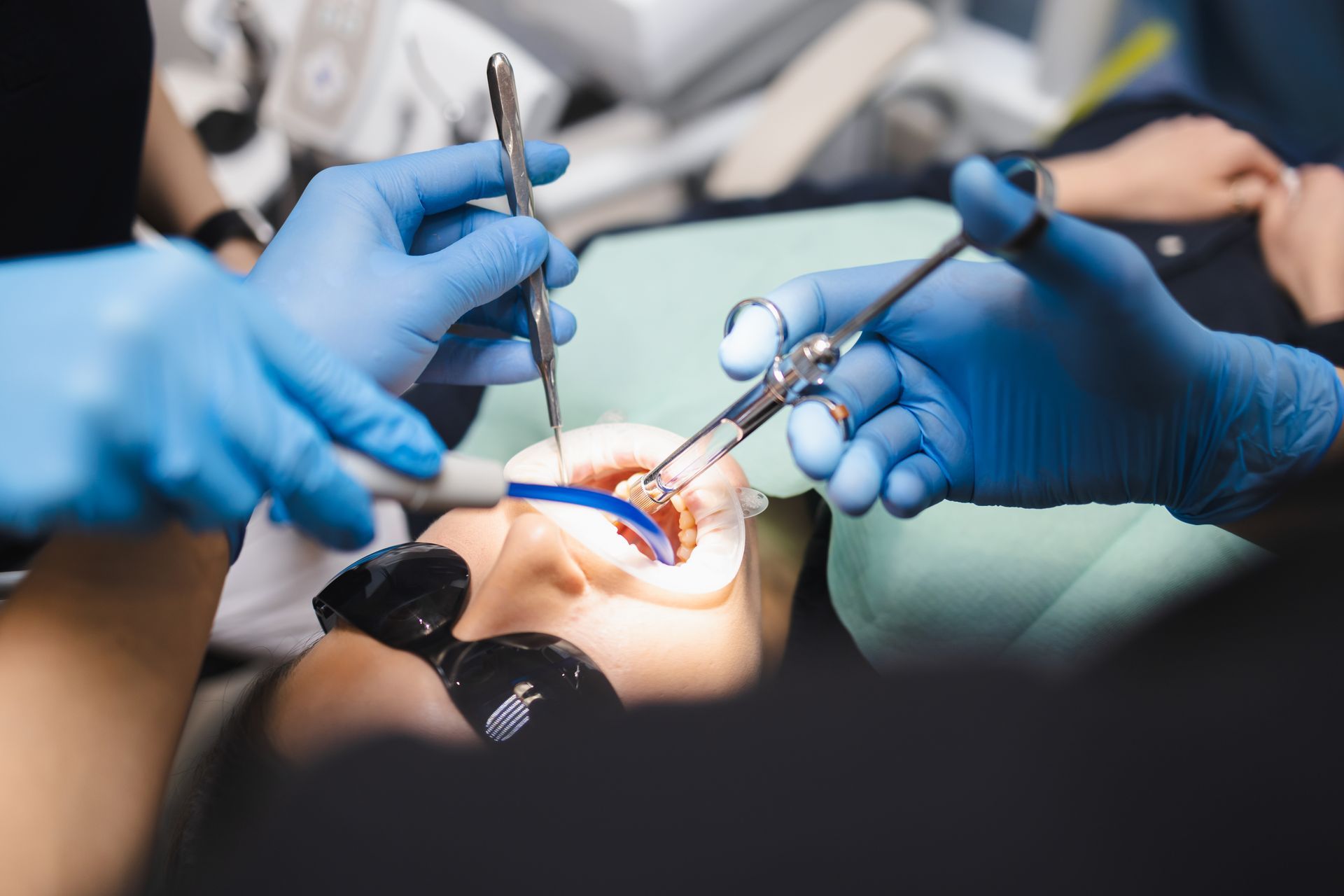
Numbing the Area
Your dentist will administer a local anesthetic to fully numb the tooth and surrounding tissue before the procedure begins. You should feel pressure during treatment but no sharp pain. If you feel discomfort at any point, let your dentist know immediately so they can adjust.
Removing Infection and Cleaning the Tooth
Once the area is numb, your dentist creates a small opening in the top of the tooth to access the pulp chamber. The infected tissue is removed, and the canals are cleaned, shaped, and disinfected to eliminate all bacteria. This is the core of the procedure.
Sealing and Restoring with a Filling or Crown
After cleaning, the canals are filled with a rubber-like material called gutta-percha and sealed to prevent reinfection. A temporary or permanent filling is placed, and in most cases a dental crown is recommended afterward to protect the tooth and restore its full function.
How to Prevent Future Root Canal Problems
Daily Brushing and Flossing
Consistent oral hygiene is the most effective way to prevent the cavities and gum disease that lead to root canal problems. Brush twice a day with fluoride toothpaste and floss at least once daily to remove plaque from between teeth and along the gum line.
Routine Dental Checkups
Regular exams allow your dentist to catch small cavities, early cracks, and signs of infection before they reach the pulp. Most problems that end in root canals were detectable at an earlier, more manageable stage.
Treat Cavities Early
A small cavity treated with a simple filling today is far easier and less expensive than a root canal tomorrow. Don't put off getting cavities filled because they aren't causing pain yet. By the time a cavity hurts, it has often already progressed significantly.
Wear a Night Guard if You Grind Teeth
Grinding and clenching put extreme pressure on your teeth and can cause cracks that expose the pulp to bacteria over time. A custom night guard absorbs that force while you sleep and can prevent the kind of damage that eventually requires root canal treatment. Learn more about how night guards prevent excess wear.
Schedule an Evaluation for Root Canal Symptoms
If any of the warning signs above sound familiar, the right move is to get the tooth evaluated as soon as possible. Root canal problems don't improve on their own, and catching an infection early gives you the best chance of a straightforward, successful outcome.
Contact Casas Adobes Dentistry today to schedule an exam. Whether you need a root canal or something simpler, our team will give you a clear, honest diagnosis and walk you through every option available to you.

Frequently Asked Questions About Root Canal Symptoms
How do I know if my tooth pain means I need a root canal or just a filling?
Pain from a cavity that hasn't reached the nerve is usually triggered by specific stimuli like sweets or temperature, and it goes away quickly once the trigger is removed. Root canal pain tends to linger after the trigger is gone, throbs on its own, or is present even without any obvious trigger. A dental exam and X-ray are the only reliable way to know for sure, but persistent or spontaneous pain is the key distinction.
Can a tooth that needs a root canal stop hurting on its own?
Yes, temporarily. If the nerve inside the tooth dies, the pain may subside. This is not a sign that the problem has resolved. The infection is still active and will continue to spread into the surrounding bone and tissue. A tooth that was painful and then suddenly stopped hurting still needs to be evaluated and treated.
Is a root canal more painful than a tooth extraction?
Most patients report that both procedures are comparable in terms of discomfort during treatment when properly numbed. Root canals have a worse reputation than they deserve. The pain associated with a root canal is usually the infection before treatment, not the procedure itself. In terms of recovery and long-term outcomes, saving a natural tooth with a root canal is almost always preferable to extraction.
How long does root canal treatment take?
Most root canals are completed in one or two appointments, each lasting between 60 and 90 minutes. More complex cases involving multiple canals or significant infection may require a second visit. Your dentist will give you a clearer timeline after evaluating the tooth.
What happens after a root canal? Do I need a crown?
After a root canal, the tooth is more brittle than a healthy tooth because it no longer has a live nerve and blood supply. A crown is recommended in most cases to protect the tooth from cracking under normal chewing pressure and to restore its full shape and function. Your dentist will advise you on whether a crown or a filling is the right option based on how much natural tooth structure remains.